Dried Blood in Ears – Toddlers Might Do This to Themselves
If you’ve ever found dried blood in your toddler’s ear, it’s likely because they stuck something in their ear and scratched the ear canal. This is a common problem among toddlers who are exploring their bodies and the world around them. While it can be worrying, it’s actually not a big deal if your child feels well and doesn’t have any other symptoms.
If it’s only dried blood – no pus, no discharge, and no pain – then there’s likely no need to see a doctor. Just clean the dried blood out of their ear with warm water. If your child is in pain, has pus or discharge, or if the dried blood won’t come out, then you should take them to see a doctor.
It Might Be an Ear Infection If Other Symptoms Are Present
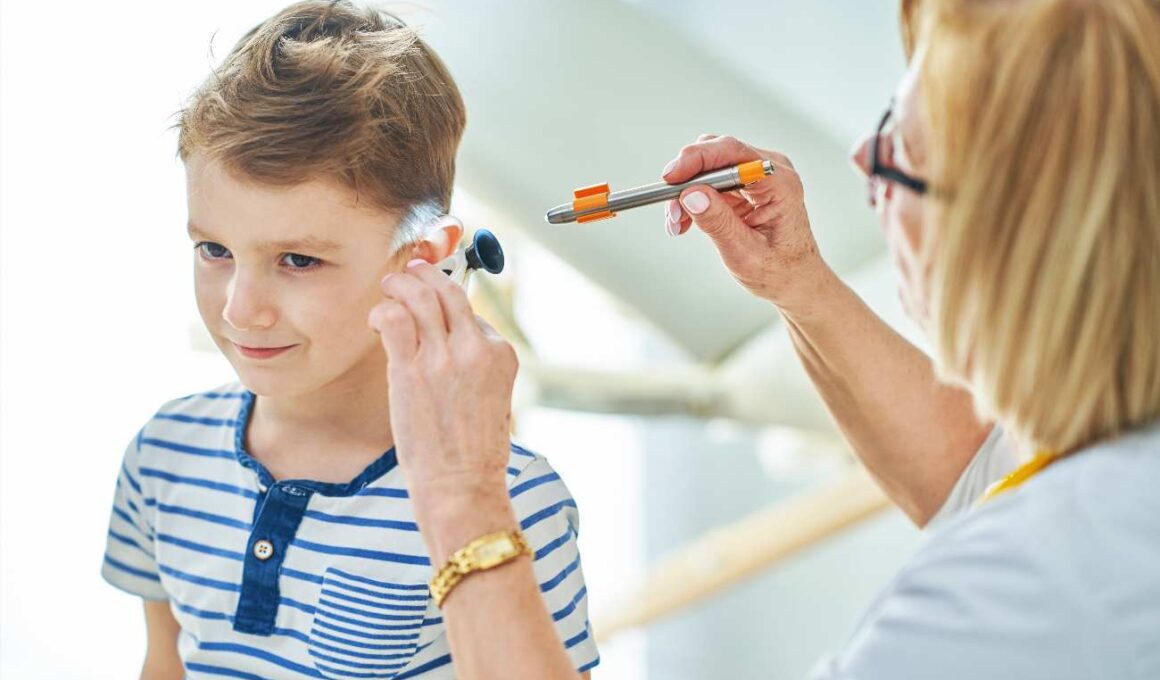
Dried blood in the ear (toddlers) can also be caused by an ear infection. If your child has other symptoms like pain, ear discharge, or fever, then it’s likely that they have an ear infection. Some other signs are:
- tugging or pulling at the ear;
- trouble sleeping;
- irritability or crankiness;
- complaining about pain in the ear;
- loss of balance;
- dizziness;
- not responding to sound;
- crust in the ear.
If your child has any of these other symptoms, then you should take them to see a doctor. Ear infections are common in young children and are usually treated with antibiotics.
Symptoms of a Ruptured Eardrum – When Things Become Serious
In rare cases, dried blood in the ear of a toddler can be a sign of a ruptured eardrum. This might have happened if your child stuck a long object in their ear or if they had a head injury. A ruptured eardrum is a serious condition that needs to be seen by a doctor. Some symptoms of a ruptured eardrum are:
- severe pain in the ear;
- bleeding from the ear;
- a feeling of fullness in the ear;
- tinnitus (ringing in the ear);
- vertigo (feeling like you’re spinning).
If your child has any of these symptoms, then you should take them to see a doctor right away. Treating a ruptured eardrum usually involves a course of antibiotics (if there is infection) and pain relief. The eardrum should heal on its own within a few weeks, but sometimes, a procedure might be necessary to close the hole.
What Should the Doctor Know?
When you take your child to see the doctor, there are a few things they will want to know. It’s important to be honest with the doctor so that they can give your child the best possible care. Be sure to tell the doctor:
- how long has it been since you noticed the dried blood in their ear;
- if your child has had any head injuries;
- if your child has been sticking anything in their ear;
- if there are any other symptoms present;
- if your child has had any ear infections in the past;
- if anyone in your family has had any ear problems.
The doctor will also want to know about your child’s medical history and will likely do a physical examination. They might also need to order some tests, like an X-ray, to rule out any other problems.
Preventing Dried Blood in Ears (Toddlers)
There are several ways to prevent dried blood in ears. Toddlers should be taught not to stick anything in their ears. If they do, then you should closely monitor them to make sure they don’t cause any damage. It’s also important to keep their nails short so that they can’t scratch their ear canal.
If your child has a history of ear infections, then you should talk to your doctor about ways to prevent them. Some ear infections can be prevented with vaccinations (like the flu vaccine). You should also make sure to treat any cold or respiratory infection promptly, as these can lead to ear infections.
Now you know what causes dried blood in ears. Toddler curiosity is the most likely culprit, but it can also be caused by an ear infection. If your child has any other symptoms, then you should seek medical attention as soon as possible.
Similar Posts:
- Toddler Covering Ears – Pain, Defiance or What?
- Should I Be Worried About My Child’s Red Poop? Toddler Health Guide
- Mucus in Toddler Poop: Causes of Mucus in Baby Stool
- Toddler Tilts Head to One Side Occasionally – Is Head Tilting Normal?
- Green Poop – Toddler Care, Treatment and Causes of Green Stool in Kids